Practice change initiatives
This program aims to empower local leaders to change their practice to provide treatment for inpatients that is appropriate for their level of frailty.
In hospitals, many frail patients are managed by clinicians with expertise in single-system problems. Clinical Practice Guidelines are usually based on evidence from trials recruiting middle-aged patients at the fitter end of the health spectrum, without co-morbidities or cognitive/psychosocial problems. Application of these guidelines can result in hospital-acquired complications for frail patients.
This program of research involves:
- conducting detailed analyses to understand the impact of frailty on outcomes based on specific interventions and/or illnesses in key patient groups;
- undertaking a process evaluation of barriers to, and enablers of, the application of frailty information in clinical practice. This evaluation will be guided by the CFIR (below);
- co-creating frailty information resources for patients and caregivers; and
- communicating these findings to specialists and other health care workers.
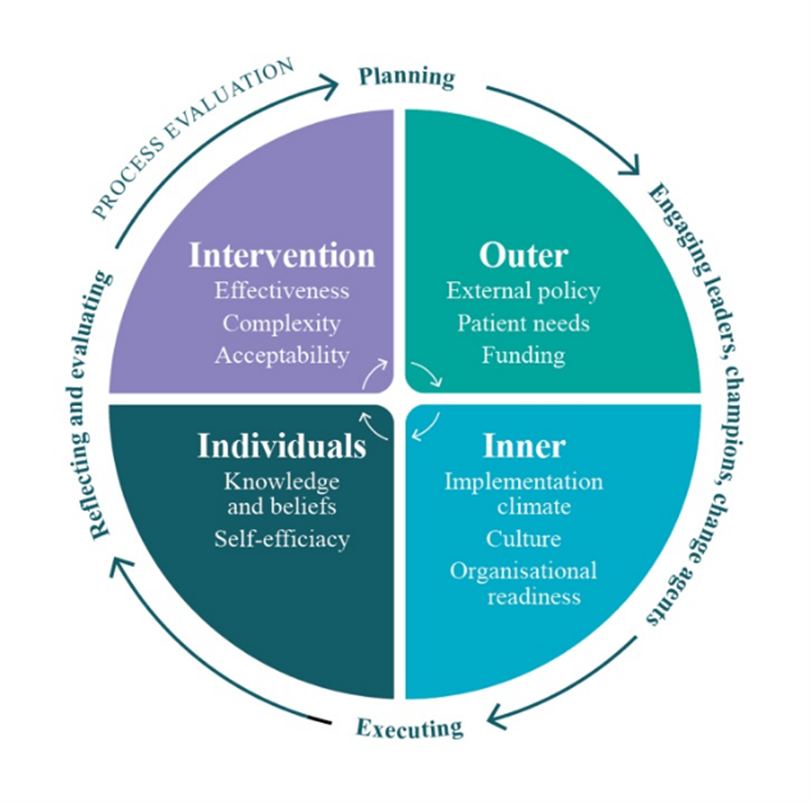
The outcomes of this research will provide a comprehensive understanding of the risk of adverse outcomes for specific treatments or illnesses that occur in hospitals. This new knowledge will be transferred to policy and practice by championing practice change initiatives.
This research program is led by Professor Monika Janda from the University of Queensland.
